Prevention of angiogenesis using prosthetic material interposition on the crossectomy stump in variscose vein recurrence surgery : 149 operations

Prevention of angiogenesis using prosthetic material interposition on the crossectomy stump in variscose vein recurrence surgery : 149 operations
SUMMARY
A study of 211 patients undergoing inguinal revision surgery for recurrence of varices of the great saphenous Vein enabied us to define two types of recurrence : Hemodynamictype recurrences that can be surgically controlled, whereby in 62% of cases a major residual inguinal reflux and a residual crural saphenous vein are associated; and angiogenetic-type recurrences associated in 57% of cases with microscopie femorovariceal neojunction as well as diffuse varicosis. Implantation of a Gore-Tex ePTFE patch on the femoral stump to reduce the risk of recurrence seemed to be an innovative way of isolating the sapheno-femoral stump from sub-cutaneous tissues.
The low morbidity of such technique as practised on 149 consecutive cases shows it to be an additional means of preventing the risk of recurrent varicosis of the great saphenous vein following surgery.
INTRODUCTION
Surgery of the greater saphenous vein is unfortunately associated with a high rate of recurrence (Tab I). In our series we performed 211 inguinal revisions to delete the femoro-variceal neojunction. The anatomical study of the revision surgery permitted us to design a surgical procedure to curb the risks of recurrence.
TABLE 1 : FREQUENCY OF RECURRENT VARICOSE VEINS AFTER STRIPPING OF THE GREAT SAPHENOUS VEIN
| Reference | year | % (n) | recurrence | followup |
| RILVIN | 1975 | 6 % 1708 | clinical recurrence | 5-10 yrs |
| JACOBSEN | 1979 | 10 % 161 | clinical recurrence | 3 yrs |
| MUNN | 1981 | 36 % 57 | clinical recurrence | 3-4 yrs |
| ROYLE | 1986 | 18 % 367 | clinical recurrence | 5 yrs |
| HAMMERSTEN | 1990 | 12 % 24 | clinical recurrence | 5 yrs |
| LAURIKKA | 1994 | 12 % 164 | clinical recurrence surgical revision |
10 yrs |
MATERIAL AND METHOD
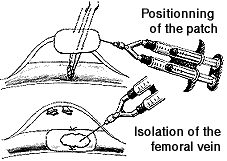
Patients with recurrent varicosities of the great saphenous veins underwent a pulsedprobe Doppler ultrasonography to detect the presence of a residual reflux in the groin and of a residual saphenous vein segment in the thigh. 211 consecutive examinations were performed . Preoperative examination of anatomical structures made it possible to define a » major reflux » as being an large reflux associated with a large residual branch of the junction and a « minor reflux on angiogenesis » as being a minimum reflux involving some tortuous veins. During this stretch of exploration, once patient n¡ 62 had been examined and operated on, we elected to principally interpose inert material in front of the stump left from the old crossectomy. This procedure (Figure 1) was carried out in the course of 149 consecutive operations that involved operating again at the previous crossectomy site. Locoregional anesthesia was performed with lidocaine and the femoral block controlled through electrical stimulation. A slantwise incision was made upward and externally over a length of 4 to 5 cm, beginning at the level of the femoral stump from the previous crossectomy. The vascular sheath was opened and the femoral vein dissected by upward lifting of the prevascular lamina.
The residual stump was often found to be located on the anteromedial side of the femoral vein. Once the stump had been ligated with Ercedex, external traction was then applied to the branches of the parietal junction, (whether external, pudental or crual). These branches were then ligated by means of 4.0 Prolene wire or a clip. Any residual saphenous branch was held in place with forceps or thread before being stripped by invagination. Any endothelium present on the stump was micro-coagulated and stitches of 4.0 Prolene wrapped around the stump.
Depending on the patient’s anatomy, obliteration of the residual stump may be effected in two ways.
- By lateral femoral clamping and complete resection of the stump followed by a continuous 6-0 Prolene wire suture.
- By putting a transverse suture for burying the stump into the venous adventia in order to prevent any connection from forming between the endothelial cells of the stump’s lumen and subcutaneous tissues
In each case, by placing an ePTFE membrane , 1 centimeter thick, on the stump, a barrier was erected between the femoral stump and the subcutaneous tissues. This patch was trimmed to about 2 to 3 cm2, approximately 2 cm in length and 1 cm in width, placed over the femoral stump so as to greatly overlap the suture site, anchored with two Prolene stitches and glued in place with biological glue. The incision was then closed by means of a slow-resorbing intradermal suture.
Figure 1
Resection of the residual stump
Suppression of the stump
RESULTS
The operation, performed on an outpatient basis, involved 134 patients ; 15 of them were hospitalized, either for personal reasons or because of an adverse social environment or medical problems such as : postoperative asthenia, too long a period of anesthesia, or intercurrent
disorders mainly affecting the nose and throat. All patients were reexamined 45 days after the operation; Doppler ultrasound examination did not reveal any collection of fluid nor any deformation of the venous femoral wall.
Twice during the operation, a lateral tear in the femoral vein, caused by disinsertion of one branch prevented us from applying the patch. One of the patients, who was obese, complained of chest pain a few hours after the operation. He was admitted to the hospital for cardiopulmonary observation which did not reveal the presence of any thromboembolic complications.In 2 cases, there was a delay in scarring (2 weeks). Infectious complications were recorded in 4 other cases
(one abscess had to be drained under general anesthesia at day 8 postoperatively, but did not require removal of the patch). One case presented with an hematoma which was spontaneously evacuated without infections complications. In all cases tolerability of the patch was high and no rejection occurred. No lymphorrhea was observed postoperatively.
DISCUSSION
Study of those various anatomical features associated with recurrent varicose veins showed this condition to be caused by two mechanisms [1]
- Histological recurrences, e.g., diffuse varicosities without residual reflux, in which the recurrence is attributable to angiogenetic biological phenomena [2].
- Mechanical recurrences in which residual hemodynamic hyperpressure appears to be a key factor in explaining recurrence is actually due to mistakes.
It follows that in order to prevent recurrence following complete crossectomy, potential connections between the femoral vein and the superficiel subcutaneous tissues should be avoided [3-4]. Prefemoral isolation has been suggested for first-line crossectomy by suturing the cribiform fascia in front of the femoral vein [4]. Implanting prosthetic material in front of the vein has also been suggested for the surgical cure of short [5] saphenous vein reflux.Since the fascia cannot be sutured in front of the vein in revision surgery following recurrences, we elected to use a sheet of Gore-Tex sheet surgical membrane. The low porosity of the ePTFE patch (under one µ), which is used for pericardial [6] or peritoneal reconstruction, seemed worthy of consideration to prevent any cellular ingrowth.
A cutaneous incision, placed a little further away from the patch implantation site, may also minimize the risk of postoperative infection.
REFERENCES
- CRETON D. Hypothèses étiologiques des récidives variqueuses Saphène internes : Etude anatomique sur 211 cas. Phlebology’95, D Negus et al. (eds).Phlebology (1995). Suppl. 1, 164-168.
- COUFFINHAL JC, BOUCHEREAU R. Angiogénèse et insuffisance veineuse superficielle ‘la maladie induite’. Phlébologie, 1990; 43: 609-613.
- GLASS GM. Prevention and recurrent saphenofemoral incompetence after surgery for varicose veins, Br J Surg, 1989; 76: 1210
- SHEPPARD M. The incidence diagnosis and management of sapheno-popliteal incompetence, Phlebology, 1986; 1: 23-32
- AMATO JJ, COTRONEO JV, GALDIERI RJ, ALBOLIRAS E, ANTILLON J, VOGEL RL. Experience with the Surgical Membrane for Pericardial Closure in Operations for Congenital Cardiac Defects. J Thorac Cardiovasc Surg 1989; 97: 929-934.
| Date | 1996 |
| Auteurs | In: MONDUZZI, eds. international congress of phlebology Corfou, BOLOGNE, 1996, 103-107 D. CRETON EC Ambroise Paré, rue Ambroise Paré 54100 F-NANCY |






