Study of the limits of local anesthesia in one- day surgery in the case of 1500 strippings of the great saphenous vein

Study of the limits of local anesthesia in one- day surgery in the case of 1500 strippings of the great saphenous vein
Summary
An evolutive study over 5 years and 1500 great saphenous vein strippings under local anesthesia in ambulatory surgery show that today all these operations can be carried out under local anesthesia ( by femoral block and injection of LIDOCAINE).
90 % can be carried out in one-day surgery on condition that post-operatory pain is reduced by using certain techniques ( invagination stripping, phlebectomy with Muller hook) and that operatory risks, especially thrombo-embolic, are reduced and that post-operatory care at home is facilitated. Factors limiting ambulatory surgery are those of environment and the seriousness of the varicosed veins
After 5 years experience and 1500 operations on varicosed veins involving strippings of the great saphenous vein in one-day surgery, we were interested to know the limits of local anesthesia and ambulatory surgery for this operation.
Haut de page Materials
The study covers a 5 year period, from 1988 to 1992, divided into 5 equal parts.
The operation was performed in the same clinic and in the same way, all the patients were seen at least 21 days after the operation. All patients had idiopathie varicosed veins.
Description of the technique
1 ) The operation consists of :
- a crossectomy with dissection of the femoral vein by a 4 cm incision in the pubic triangle above and inside the inguinal fold.
- Access to the great saphenous vein below the lower side of the malleolus by an incision of 5 or 10 mm.
- Stripping by downward invagination.
- Where necessary, an short saphenous vein crossectomy and short saphenous vein stripping by invagination.
- Superficial phlebectomies, using the Muller hook with complete ablation of the varicosed network ( saphenous branches and perforating veins, with incisions of 1 to 2 mm ( average number of incisions per operation is 30).
- Intra dermic thread (Polyglactine ) is used for the sutures, at the top and the bottom of the stripping, ; the knot is inside.
- A continuous aspiration drain is placed the length of the stripping during the operation.
- The bandage is in two parts :
- Firstly a fixed elastic bandage is put on for 5 days, necessary for the decubitus position.
- Secondly, a removable elastic bandage is put on over this, when standing or walking.
- The operation lasts about 1 hour.
- The dressing and the steristrips are removed at home by a nurse.
2 ) The anesthesia is prepared before the operation.
- Pre-operatory medication is given on request with 25 mg to 150 mg HYDROXYZINE.
- A femoral block with neurological research by electrostimulation is carried out by injection of LIDOCAINE 1 % with or without ADRENALINE. Electrostimulation not only locates the main branch of the common trunk but also the sensitive branches of the femoral nerve : internal and medial femoro cutaneous nerve, by sub-cutaneous fasciculations and the areas of paresthesia felt by the patient. This helps to increase the precision of the femoral block. The volume of the injection is from 5 to 10 ml.
- Complementary injections necessary for cutaneous anesthesia above the limits of the femoral block are carried out with LIDOCAINE , diluted to 0,75 or 0,5 with bicarbonate.
- We do not carry out a sciatic block , for the vasoplegia induced by a sciatic block makes the operation less precise. Vasoplegia rarely occurs with a femoral block.
- An injection of 1 to 5 mg of MIDASOLAN an 0,5 to 1,5 mg of ALFINTANYL is given during the operation, depending on the psychological state of the patient.
- The anesthesia is prepared 30 minutes to 1 hour before the operation.
- The average volume of local anesthesia per operation is 44 ml.
- The patient is treated for 8 days with low molecular weight HEPARINE.
Limits of local anesthesia
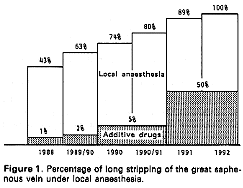
Since 1988 the percentage of operations carried out under local anesthesia has increased regularly. From 43 % in 1988 , it is now 100 % these last two years. Table 1 .This means that there is, at the moment, no contra-indication to local anesthesia.
We use only 44 ml of product for a complete operation, thus leaving a high margin for complementary injections, which increase the anesthetised surface, necessary, for instance, for patients with large numbers of varicosed veins, requiring 130 incisions for a complete operation.
Obesity is not an obstacle to local anesthesia. We have operated patients weighing up to 160 kilos. Minimal post-operatory bleeding and the mobility of the patient facilitate the operation.
We have also carried out strippings of the great and short saphenous veins simulataneously in 6 % of cases.
We strongly encourage patients to choose local anesthesia as we are convinced that it ameliorates the surgery results. And now in 50 % of cases we inject additive anxiolitic drugs l. These 50 % certainly represent the percentage of patients who would not have spontaneously chosen local anesthesia.
Limits of ambulatory surgery
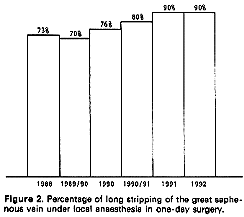
the percentage of operations under local anesthesia in one-day surgery is increasing regularly. In 1988 it was 73 % , it is now 90 % since the last two years. table 2
Of the remaining 10 % of patients who did not undergo one-day surgery, it can be seen that 50 % were patients who would not , or could not be operated on in ambulatory conditions for medical reasons : diabetes, anti-coagulant treatment, patient currently hospitalised , inter-current disease, or for non -medical reasons : comfort, psychological problems , no help at home, transport problems, bad weather, or living too far away.
In fact, only 5 ,% of patients were actually unable to have one-day surgery. These were often elderly patients with many varicosed veins ( more than forty incisions), with sub-cutaneous lesions, varicose ulcer scars, and those where the operation was carried out too late in the day to enable them to return home.
The femoral block lasts 3 to 6 hours. On three occasions, the block has lasted more than 12 hours. Only two patients have had operatory incidents prohibiting their return home : one who had a seizure during the femoral block and one with immediate post-operative bleeding on the crossectomy incision ( external pudental artery).
The rare consultations made during the first post-operative days have always been for problems related to the dressings or for hematomas of the upper part of the thigh beetwenn the groin and the elastic bandage. No re-hospitalisation has been necessary after the patient has returned home.
One-day surgery is possible in 90 % of cases for three reasons :
- The dressings and post-operatory care are extremely simple. The bandage is put on definitively on leaving the operation theatre, it does not affect physical activity at home. Out of 800 patients,70 % stated they took up normal domestic activities the day after the operation, 20 % in 4 days and 10 % after 8 days.
The bandage can be removed by the patient him/herself. - The operation causes little post -operatory pain :
- Firstly due to Muller’s phlebectomy – the tiny incisions are practically painless after the operation.
- The crossectomy incision made in the pubic triangle is in a fixed area, less painful when moving the leg.
- The lower incision acceding to the initial part of the great saphenous vein is in an area that is not exposed to bruising by the shoe, situated above the terminal division of the saphenous nerve6 ; injury during the operation is less frequent at this level.
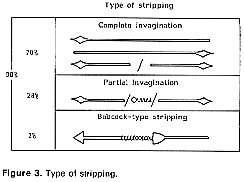
Post-operational pain is reduced when stripping is by invagination. We habe been able to use this method in 98 % of cases – either totally in 70 % of cases (downwards, upwards or in both directions with a rupture in the middle) or on three quarters of the leg in 28 % of cases ( with a vein telescoping at the level of the knee in the 25 % of the great saphenous vein) Table 3.
We have been obliged to carry out a classical Backok-type[1] stripping in only 2 % of the cases.
Local anesthesia and continous aspiration over the whole length of stripping throughout the operation until the dressing has been done, diminishes hematomas and post-operatory pain.
Finally, by using the invagination method of stripping we are able to avoid any neurological lesions to the saphenous nerve, which greatly reduces the risk of post- operational pain. In fact, it is known that Backok stripping under general anesthesia can cause damage to the saphenous nerve in 30 to 50 % of cases, depending on the direction of the stripping.[24578]
We have already shown3 that there is a 1,2 % risk of injury to the great saphenous nerve during stripping by invagination under general anesthesia and that when this same invagination stripping is carried out under local anesthesia, these neurological lesions can be completely avoided when the patient starts to feel a specific « muscular cramp » type pain when the saphenous nerve is stretched in the loop of the invagination .
1. We have been able to considerably reduce post-operative risks, especially thrombo-embolic risks. We have never had any thrombo-embolic complications in the 1500 operations carried out under local anesthesia in one-day surgery. This can be attributed to the absence of vasoplegia and a concommitant acceleration of deep circulation.
The only problem we have had – that is one out of four hundred patients – concerned a young patient hospitalised for 2 days. The pulmonary emboly which occurred on the 8 th day cleared up without after-effects. This represents 2,5 per thousand among the hospitalised patients.
Haut de page Geographical limits of one-day surgery
This one-day surgery is widely regional :
21 % of patients live in Nancy or in the close surroundings
74 % of patients are uniformly scattered up to 110 km
4 % live further away, up to a maximum of 230 km
After leaving the centre, supervision at home by telephone through the nurse or general practitioner is useful especially to reassure the patient on the normal evolution of the healing process.
Haut de page Conclusion
1. The certainty of being able to improve the results of varicose excision surgery by using local anesthesia has made us extend progressively to all of our patients our indications on local anesthesia.
As a matter of fact , local anesthesia diminishes peroperatory bleeding and postoperatory bruising which permits patients to put themselves in the best position for facilitating the operation and, makes it possible (in spite of the femoral block) to avoid any neurological traumatism in the area of the popliteal space and at the saphenous nerve during stripping and, lastly to diminish the risk of thrombo-embolic complication.
Local anesthesia by the persistance of the deep proprioceptive sensation limits the agression of the operation and imposes light gestures on the surgeon which can be beneficial for the results of the operation.
The anatomical contraindications have been removed by the femoral block and by the precision of location by electrostimulation.
The psychological contra indication have been removed by using anxiolitic with a very short live very much inuse at this time.
The perception of local anesthesia for many patients depends on their contact with the anesthetist and the surgical team.
1. The augmentation of our performance of ambulatory surgery, now up to 90 % , has been accomplished spontaneously by a regular improvement in the manner or performing the operation.
- The suppression of major postoperatory risks has permitted us to reassure patients and convince them that postoperative surveillance in the hospital in not necessary.
- The diminution of postoperatory pain is the essential element which has permitted us to give our patients an immediate postoperatory autonomy, completely satisfactory, and to decrease their « pain anxiety » ( pain is the element which causes the most postoperatory anxiety).
- Simplifying prostoperatory care in the home is the last reassuring element of the intervention. The bandage is the surgeon’s signature which the patient takes home with him ; it must be comfortable and secure.
If local anesthsia can be imposed on the patient in order to improve the surgical results, ambulatory surgery should be left to the patient ‘s choice. With improvement in the operating technics and surgical environment, ambulatory surgery can be performed in 90 % of the time.
REFERENCES
- BABCOCK W.W. A new operation for the extirpation of varicose veins of the leg. N. Y. Med. J. 1907 ; 86 : 153 – 6
- COX S.J., WELWOOD J. M., MARTIN A. Saphenous nerve injury caused by stripping of the long saphenous vein . Br . Med. J., 1974 ; 1 : 415-417
- CRETON D. The results of great saphenous vein stripping under local anaesthesia in outpatient care:700 cases. Phlébologie 1991 ; 44 : 303-312
- FULLARTON GM., CALVERT MH. Intraluminal long saphenous vein stripping : a technique minimizing peri veinous tissue trauma. Br. J. Surg. 1987 ; 74 : 255
- GARNJOBST W. Injuries to the saphenous nerve following operations for varicose veins. Surg. Gynecol. Obstet. 1964 ; 119 ; 359-361
- HOLME J.B, HOLME K., SORENSEN L.S. The anatomic relationship between the long saphenous vein and the saphenous nerve . Acta. Chir. Scand. 1988 ; 154 : 631-633
- RAMASASTRY S.S ., DICK G., FUTRELL J. W. Anatomy of the saphenous nerve : relevance to saphenous vein stripping . Am. Surgeon. 1987 ; 53 : 274-277.
- STAELENS. I., VAN DER STRICHT J., Complication rate of long stripping of the greater saphenous vein. Phlebology 1992 ; 7 : 67-70
| Date | 1993 |
| Auteurs | Ambulatory Surgery 1993 ; 1 : 132-135 D. CRETON EC. Ambroise Paré, rue Ambroise Paré 54100 F-NANCY |



